- Adrenal gland
- 2023 Korean Endocrine Society Consensus Guidelines for the Diagnosis and Management of Primary Aldosteronism
-
Jeonghoon Ha, Jung Hwan Park, Kyoung Jin Kim, Jung Hee Kim, Kyong Yeun Jung, Jeongmin Lee, Jong Han Choi, Seung Hun Lee, Namki Hong, Jung Soo Lim, Byung Kwan Park, Jung-Han Kim, Kyeong Cheon Jung, Jooyoung Cho, Mi-kyung Kim, Choon Hee Chung, The Committee of Clinical Practice Guideline of Korean Endocrine Society, The Korean Adrenal Study Group of Korean Endocrine Society
-
Endocrinol Metab. 2023;38(6):597-618. Published online October 13, 2023
-
DOI: https://doi.org/10.3803/EnM.2023.1789
-
-
3,459
View
-
483
Download
-
1
Web of Science
-
1
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
- Primary aldosteronism (PA) is a common, yet underdiagnosed cause of secondary hypertension. It is characterized by an overproduction of aldosterone, leading to hypertension and/or hypokalemia. Despite affecting between 5.9% and 34% of patients with hypertension, PA is frequently missed due to a lack of clinical awareness and systematic screening, which can result in significant cardiovascular complications. To address this, medical societies have developed clinical practice guidelines to improve the management of hypertension and PA. The Korean Endocrine Society, drawing on a wealth of research, has formulated new guidelines for PA. A task force has been established to prepare PA guidelines, which encompass epidemiology, pathophysiology, clinical presentation, diagnosis, treatment, and follow-up care. The Korean clinical guidelines for PA aim to deliver an evidence-based protocol for PA diagnosis, treatment, and patient monitoring. These guidelines are anticipated to ease the burden of this potentially curable condition.
-
Citations
Citations to this article as recorded by  - Correlation of Histopathologic Subtypes of Primary Aldosteronism with Clinical Phenotypes and Postsurgical Outcomes
Chang Ho Ahn, You-Bin Lee, Jae Hyeon Kim, Young Lyun Oh, Jung Hee Kim, Kyeong Cheon Jung
The Journal of Clinical Endocrinology & Metabolism.2023;[Epub] CrossRef
- Adrenal Gland
- Metabolic Subtyping of Adrenal Tumors: Prospective Multi-Center Cohort Study in Korea
-
Eu Jeong Ku, Chaelin Lee, Jaeyoon Shim, Sihoon Lee, Kyoung-Ah Kim, Sang Wan Kim, Yumie Rhee, Hyo-Jeong Kim, Jung Soo Lim, Choon Hee Chung, Sung Wan Chun, Soon-Jib Yoo, Ohk-Hyun Ryu, Ho Chan Cho, A Ram Hong, Chang Ho Ahn, Jung Hee Kim, Man Ho Choi
-
Endocrinol Metab. 2021;36(5):1131-1141. Published online October 21, 2021
-
DOI: https://doi.org/10.3803/EnM.2021.1149
-
-
5,100
View
-
209
Download
-
8
Web of Science
-
8
Crossref
-
 Abstract Abstract
 PDF PDF Supplementary Material Supplementary Material PubReader PubReader  ePub ePub
- Background
Conventional diagnostic approaches for adrenal tumors require multi-step processes, including imaging studies and dynamic hormone tests. Therefore, this study aimed to discriminate adrenal tumors from a single blood sample based on the combination of liquid chromatography-mass spectrometry (LC-MS) and machine learning algorithms in serum profiling of adrenal steroids.
Methods
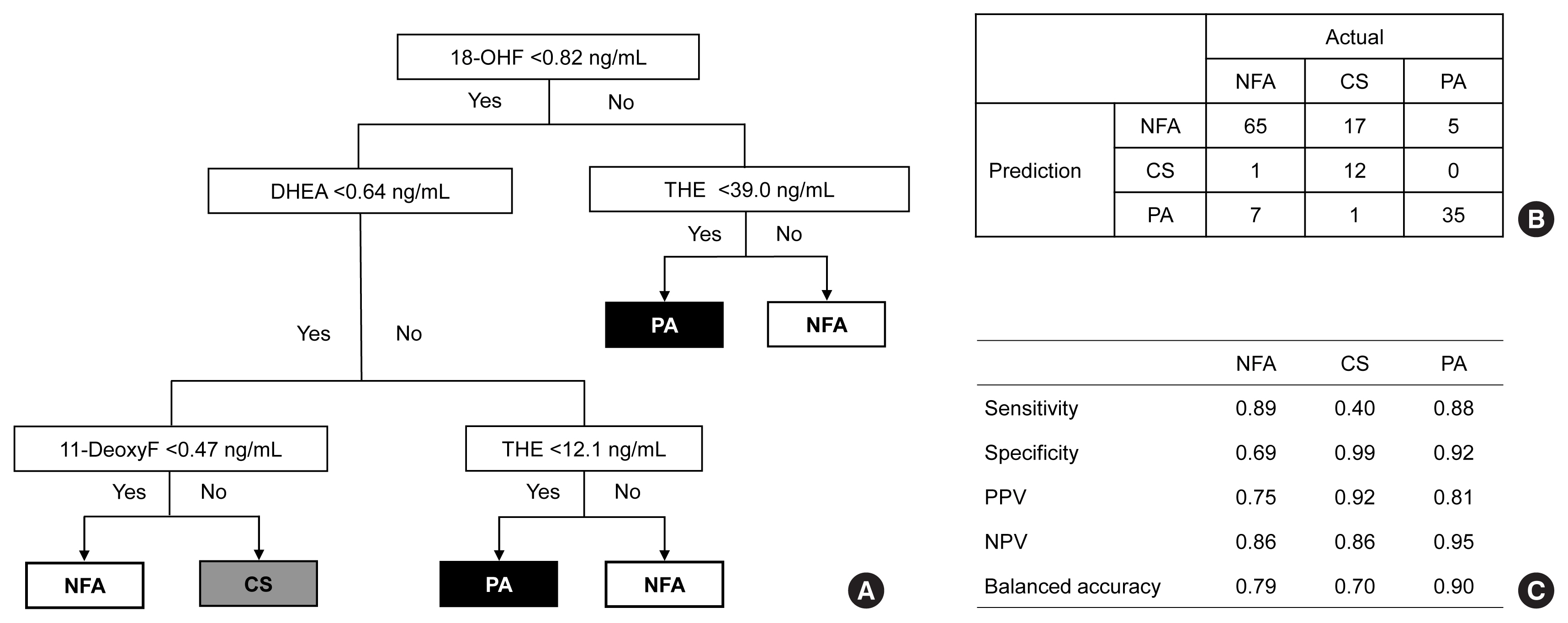
The LC-MS-based steroid profiling was applied to serum samples obtained from patients with nonfunctioning adenoma (NFA, n=73), Cushing’s syndrome (CS, n=30), and primary aldosteronism (PA, n=40) in a prospective multicenter study of adrenal disease. The decision tree (DT), random forest (RF), and extreme gradient boost (XGBoost) were performed to categorize the subtypes of adrenal tumors.
Results
The CS group showed higher serum levels of 11-deoxycortisol than the NFA group, and increased levels of tetrahydrocortisone (THE), 20α-dihydrocortisol, and 6β-hydroxycortisol were found in the PA group. However, the CS group showed lower levels of dehydroepiandrosterone (DHEA) and its sulfate derivative (DHEA-S) than both the NFA and PA groups. Patients with PA expressed higher serum 18-hydroxycortisol and DHEA but lower THE than NFA patients. The balanced accuracies of DT, RF, and XGBoost for classifying each type were 78%, 96%, and 97%, respectively. In receiver operating characteristics (ROC) analysis for CS, XGBoost, and RF showed a significantly greater diagnostic power than the DT. However, in ROC analysis for PA, only RF exhibited better diagnostic performance than DT.
Conclusion
The combination of LC-MS-based steroid profiling with machine learning algorithms could be a promising one-step diagnostic approach for the classification of adrenal tumor subtypes.
-
Citations
Citations to this article as recorded by  - Treating Primary Aldosteronism-Induced Hypertension: Novel Approaches and Future Outlooks
Nathan Mullen, James Curneen, Padraig T Donlon, Punit Prakash, Irina Bancos, Mark Gurnell, Michael C Dennedy
Endocrine Reviews.2024; 45(1): 125. CrossRef - Steroid profiling in adrenal disease
Danni Mu, Dandan Sun, Xia Qian, Xiaoli Ma, Ling Qiu, Xinqi Cheng, Songlin Yu
Clinica Chimica Acta.2024; 553: 117749. CrossRef - Serum and hair steroid profiles in patients with nonfunctioning pituitary adenoma undergoing surgery: A prospective observational study
Seung Shin Park, Yong Hwy Kim, Ho Kang, Chang Ho Ahn, Dong Jun Byun, Man Ho Choi, Jung Hee Kim
The Journal of Steroid Biochemistry and Molecular Biology.2023; 230: 106276. CrossRef - Recent Updates on the Management of Adrenal Incidentalomas
Seung Shin Park, Jung Hee Kim
Endocrinology and Metabolism.2023; 38(4): 373. CrossRef - LC-MS based simultaneous profiling of adrenal hormones of steroids, catecholamines, and metanephrines
Jongsung Noh, Chaelin Lee, Jung Hee Kim, Seung Woon Myung, Man Ho Choi
Journal of Lipid Research.2023; 64(11): 100453. CrossRef - 2023 Korean Endocrine Society Consensus Guidelines for the Diagnosis and Management of Primary Aldosteronism
Jeonghoon Ha, Jung Hwan Park, Kyoung Jin Kim, Jung Hee Kim, Kyong Yeun Jung, Jeongmin Lee, Jong Han Choi, Seung Hun Lee, Namki Hong, Jung Soo Lim, Byung Kwan Park, Jung-Han Kim, Kyeong Cheon Jung, Jooyoung Cho, Mi-kyung Kim, Choon Hee Chung
Endocrinology and Metabolism.2023; 38(6): 597. CrossRef - Toward Systems-Level Metabolic Analysis in Endocrine Disorders and Cancer
Aliya Lakhani, Da Hyun Kang, Yea Eun Kang, Junyoung O. Park
Endocrinology and Metabolism.2023; 38(6): 619. CrossRef - Prevalence and Characteristics of Adrenal Tumors in an Unselected Screening Population
Ying Jing, Jinbo Hu, Rong Luo, Yun Mao, Zhixiao Luo, Mingjun Zhang, Jun Yang, Ying Song, Zhengping Feng, Zhihong Wang, Qingfeng Cheng, Linqiang Ma, Yi Yang, Li Zhong, Zhipeng Du, Yue Wang, Ting Luo, Wenwen He, Yue Sun, Fajin Lv, Qifu Li, Shumin Yang
Annals of Internal Medicine.2022; 175(10): 1383. CrossRef
- Miscellaneous
- Diagnosis and Treatment of Growth Hormone Deficiency: A Position Statement from Korean Endocrine Society and Korean Society of Pediatric Endocrinology
-
Jung Hee Kim, Hyun Wook Chae, Sang Ouk Chin, Cheol Ryong Ku, Kyeong Hye Park, Dong Jun Lim, Kwang Joon Kim, Jung Soo Lim, Gyuri Kim, Yun Mi Choi, Seong Hee Ahn, Min Ji Jeon, Yul Hwangbo, Ju Hee Lee, Bu Kyung Kim, Yong Jun Choi, Kyung Ae Lee, Seong-Su Moon, Hwa Young Ahn, Hoon Sung Choi, Sang Mo Hong, Dong Yeob Shin, Ji A Seo, Se Hwa Kim, Seungjoon Oh, Sung Hoon Yu, Byung Joon Kim, Choong Ho Shin, Sung-Woon Kim, Chong Hwa Kim, Eun Jig Lee
-
Endocrinol Metab. 2020;35(2):272-287. Published online June 24, 2020
-
DOI: https://doi.org/10.3803/EnM.2020.35.2.272
-
-
9,478
View
-
428
Download
-
13
Web of Science
-
15
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
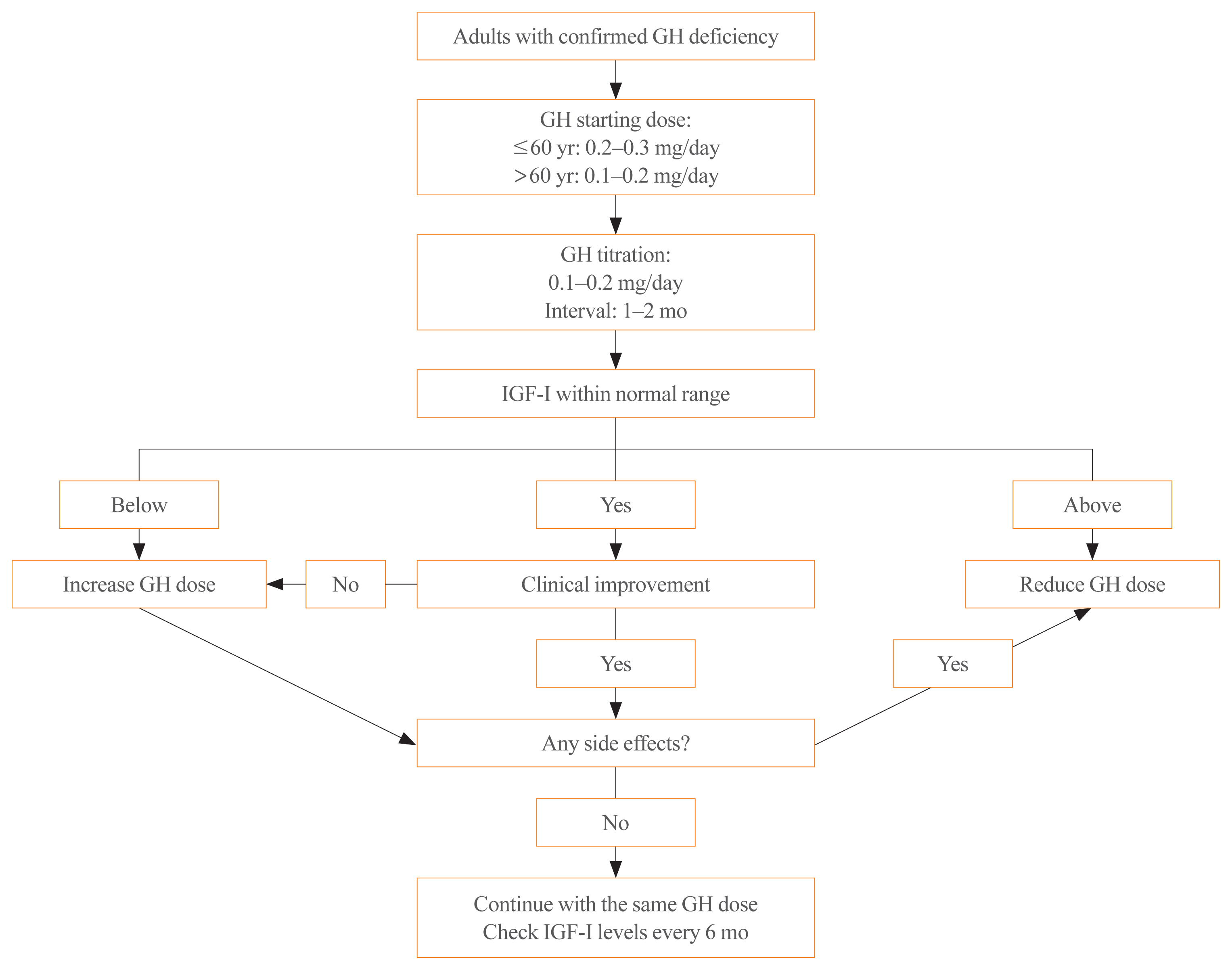
- Growth hormone (GH) deficiency is caused by congenital or acquired causes and occurs in childhood or adulthood. GH replacement therapy brings benefits to body composition, exercise capacity, skeletal health, cardiovascular outcomes, and quality of life. Before initiating GH replacement, GH deficiency should be confirmed through proper stimulation tests, and in cases with proven genetic causes or structural lesions, repeated GH stimulation testing is not necessary. The dosing regimen of GH replacement therapy should be individualized, with the goal of minimizing side effects and maximizing clinical improvements. The Korean Endocrine Society and the Korean Society of Pediatric Endocrinology have developed a position statement on the diagnosis and treatment of GH deficiency. This position statement is based on a systematic review of evidence and expert opinions.
-
Citations
Citations to this article as recorded by  - Once-Weekly Somapacitan as an Alternative Management of Growth Hormone Deficiency in Prepubertal Children: A Systematic Review and Meta-Analysis of Randomized Controlled Trial
Ghina Tsurayya, Cut Alifiya Nazhifah, Muhammad Rahmat Pirwanja, Putri Oktaviani Zulfa, Muhammad Raihan Ramadhan Tatroman, Fajar Fakri, Muhammad Iqhrammullah
Children.2024; 11(2): 227. CrossRef - Evaluation of Adult Height in Patients with Non-Permanent Idiopathic GH Deficiency
Agnese Murianni, Anna Lussu, Chiara Guzzetti, Anastasia Ibba, Letizia Casula, Mariacarolina Salerno, Marco Cappa, Sandro Loche
Endocrines.2023; 4(1): 169. CrossRef - The effect of hypothalamic involvement and growth hormone treatment on cardiovascular risk factors during the transition period in patients with childhood-onset craniopharyngioma
Sang Hee Park, Yun Jeong Lee, Jung-Eun Cheon, Choong Ho Shin, Hae Woon Jung, Young Ah Lee
Annals of Pediatric Endocrinology & Metabolism.2023; 28(2): 107. CrossRef - Continuous Glucose Monitoring: A Possible Aid for Detecting Hypoglycemic Events during Insulin Tolerance Tests
Soo Yeun Sim, Moon Bae Ahn
Sensors.2023; 23(15): 6892. CrossRef - The risk patients with AGHD have of developing CVD
Eisha Javed, Maha Zehra, Naz Elahi
International Journal of Cardiology Cardiovascular Risk and Prevention.2023; 19: 200221. CrossRef - Diagnosis of GH Deficiency Without GH Stimulation Tests
Anastasia Ibba, Sandro Loche
Frontiers in Endocrinology.2022;[Epub] CrossRef - Metabolic Impacts of Discontinuation and Resumption of Recombinant Human Growth Hormone Treatment during the Transition Period in Patients with Childhood-Onset Growth Hormone Deficiency
Yun Jeong Lee, Yunha Choi, Han-Wook Yoo, Young Ah Lee, Choong Ho Shin, Han Saem Choi, Ho-Seong Kim, Jae Hyun Kim, Jung Eun Moon, Cheol Woo Ko, Moon Bae Ahn, Byung-Kyu Suh, Jin-Ho Choi
Endocrinology and Metabolism.2022; 37(2): 359. CrossRef - A Radiomics-Based Model with the Potential to Differentiate Growth Hormone Deficiency and Idiopathic Short Stature on Sella MRI
Taeyoun Lee, Kyungchul Song, Beomseok Sohn, Jihwan Eom, Sung Soo Ahn, Ho-Seong Kim, Seung-Koo Lee
Yonsei Medical Journal.2022; 63(9): 856. CrossRef - Phenotypic spectrum of patients with mutations in CHD7: clinical implications of endocrinological findings
Ja Hye Kim, Yunha Choi, Soojin Hwang, Gu-Hwan Kim, Han-Wook Yoo, Jin-Ho Choi
Endocrine Connections.2022;[Epub] CrossRef - Immune Checkpoint Inhibitors and Endocrine Disorders: A Position Statement from the Korean Endocrine Society
Hyemi Kwon, Eun Roh, Chang Ho Ahn, Hee Kyung Kim, Cheol Ryong Ku, Kyong Yeun Jung, Ju Hee Lee, Eun Heui Kim, Sunghwan Suh, Sangmo Hong, Jeonghoon Ha, Jun Sung Moon, Jin Hwa Kim, Mi-kyung Kim
Endocrinology and Metabolism.2022; 37(6): 839. CrossRef - Laron syndrome: clinic, diagnostics (а clinical case)
P.M. Lіashuk, R.P. Lіashuk, N.I. Stankova, M.B. Kudina
INTERNATIONAL JOURNAL OF ENDOCRINOLOGY (Ukraine).2022; 18(3): 193. CrossRef - Diagnosis for Pheochromocytoma and Paraganglioma: A Joint Position Statement of the Korean Pheochromocytoma and Paraganglioma Task Force
Eu Jeong Ku, Kyoung Jin Kim, Jung Hee Kim, Mi Kyung Kim, Chang Ho Ahn, Kyung Ae Lee, Seung Hun Lee, You-Bin Lee, Kyeong Hye Park, Yun Mi Choi, Namki Hong, A Ram Hong, Sang-Wook Kang, Byung Kwan Park, Moon-Woo Seong, Myungshin Kim, Kyeong Cheon Jung, Chan
Endocrinology and Metabolism.2021; 36(2): 322. CrossRef - Asian Conference on Tumor Ablation Guidelines for Adrenal Tumor Ablation
Byung Kwan Park, Masashi Fujimori, Shu-Huei Shen, Uei Pua
Endocrinology and Metabolism.2021; 36(3): 553. CrossRef - Asian Conference on Tumor Ablation guidelines for renal cell carcinoma
Byung Kwan Park, Shu-Huei Shen, Masashi Fujimori, Yi Wang
Investigative and Clinical Urology.2021; 62(4): 378. CrossRef - Diagnosis and Treatment of Adult Growth Hormone Deficiency
Jung Hee Kim
The Korean Journal of Medicine.2021; 96(5): 400. CrossRef
- Endocrine Research
- Effects of Oxytocin on Cell Proliferation in a Corticotroph Adenoma Cell Line
-
Jung Soo Lim, Young Woo Eom, Eun Soo Lee, Hyeong Ju Kwon, Ja-Young Kwon, Junjeong Choi, Choon Hee Chung, Young Suk Jo, Eun Jig Lee
-
Endocrinol Metab. 2019;34(3):302-313. Published online September 26, 2019
-
DOI: https://doi.org/10.3803/EnM.2019.34.3.302
-
-
4,998
View
-
74
Download
-
3
Web of Science
-
2
Crossref
-
 Abstract Abstract
 PDF PDF Supplementary Material Supplementary Material PubReader PubReader  ePub ePub
- Background
Oxytocin (OXT) has been reported to act as a growth regulator in various tumor cells. However, there is a paucity of data on the influence of OXT on cell proliferation of corticotroph adenomas. This study aimed to examine whether OXT affects cell growth in pituitary tumor cell lines (AtT20 and GH3 cells) with a focus on corticotroph adenoma cells. MethodsReverse transcription polymerase chain reaction and enzyme-linked immunosorbent assay were conducted with AtT20 cells to confirm the effects of OXT on hormonal activity; flow cytometry was used to assess changes in the cell cycle after OXT treatment. Moreover, the impact of OXT on proliferating cell nuclear antigen (PCNA), nuclear factor κB, and mitogen-activated protein kinase signaling pathway was analyzed by Western blot. ResultsOXT treatment of 50 nM changed the gene expression of OXT receptor and pro-opiomelanocortin within a short time. In addition, OXT significantly reduced adrenocorticotropic hormone secretion within 1 hour. S and G2/M populations of AtT20 cells treated with OXT for 24 hours were significantly decreased compared to the control. Furthermore, OXT treatment decreased the protein levels of PCNA and phosphorylated extracellular-signal-regulated kinase (P-ERK) in AtT20 cells. ConclusionAlthough the cytotoxic effect of OXT in AtT20 cells was not definite, OXT may blunt cell proliferation of corticotroph adenomas by altering the cell cycle or reducing PCNA and P-ERK levels. Further research is required to investigate the role of OXT as a potential therapeutic target in corticotroph adenomas.
-
Citations
Citations to this article as recorded by  - Increased proliferation and neuronal fate in prairie vole brain progenitor cells cultured in vitro: effects by social exposure and sexual dimorphism
Daniela Ávila-González, Italo Romero-Morales, Lizette Caro, Alejandro Martínez-Juárez, Larry J. Young, Francisco Camacho-Barrios, Omar Martínez-Alarcón, Analía E. Castro, Raúl G. Paredes, Néstor F. Díaz, Wendy Portillo
Biology of Sex Differences.2023;[Epub] CrossRef - Anterior pituitary gland synthesises dopamine from l‐3,4‐dihydroxyphenylalanine (l‐dopa)
Santiago Jordi Orrillo, Nataly de Dios, Antonela Sofía Asad, Fernanda De Fino, Mercedes Imsen, Ana Clara Romero, Sandra Zárate, Jimena Ferraris, Daniel Pisera
Journal of Neuroendocrinology.2020;[Epub] CrossRef
- Hypothalamus and Pituitary gland
- Medical Treatment with Somatostatin Analogues in Acromegaly: Position Statement
-
Sang Ouk Chin, Cheol Ryong Ku, Byung Joon Kim, Sung-Woon Kim, Kyeong Hye Park, Kee Ho Song, Seungjoon Oh, Hyun Koo Yoon, Eun Jig Lee, Jung Min Lee, Jung Soo Lim, Jung Hee Kim, Kwang Joon Kim, Heung Yong Jin, Dae Jung Kim, Kyung Ae Lee, Seong-Su Moon, Dong Jun Lim, Dong Yeob Shin, Se Hwa Kim, Min Jeong Kwon, Ha Young Kim, Jin Hwa Kim, Dong Sun Kim, Chong Hwa Kim
-
Endocrinol Metab. 2019;34(1):53-62. Published online March 21, 2019
-
DOI: https://doi.org/10.3803/EnM.2019.34.1.53
-
-
6,452
View
-
253
Download
-
8
Web of Science
-
11
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
The Korean Endocrine Society (KES) published clinical practice guidelines for the treatment of acromegaly in 2011. Since then, the number of acromegaly cases, publications on studies addressing medical treatment of acromegaly, and demands for improvements in insurance coverage have been dramatically increasing. In 2017, the KES Committee of Health Insurance decided to publish a position statement regarding the use of somatostatin analogues in acromegaly. Accordingly, consensus opinions for the position statement were collected after intensive review of the relevant literature and discussions among experts affiliated with the KES, and the Korean Neuroendocrine Study Group. This position statement includes the characteristics, indications, dose, interval (including extended dose interval in case of lanreotide autogel), switching and preoperative use of somatostatin analogues in medical treatment of acromegaly. The recommended approach is based on the expert opinions in case of insufficient clinical evidence, and where discrepancies among the expert opinions were found, the experts voted to determine the recommended approach. -
Citations
Citations to this article as recorded by  - Hydrogel-fiber-mesh-based 3D cell cultures: A new method for studying pituitary tumors
Wooju Jeong, Sungrok Wang, Yumin Kim, Soohyun Lee, Minhu Huang, Jaeil Park, Myung-Han Yoon, Chang-Myung Oh, Cheol Ryong Ku
Smart Materials in Medicine.2024;[Epub] CrossRef - Evaluation and Management of Bone Health in Patients with Thyroid Diseases: A Position Statement of the Korean Thyroid Association
A Ram Hong, Ho-Cheol Kang
Endocrinology and Metabolism.2023; 38(2): 175. CrossRef - Growth Hormone Excess: Implications and Management
Suneela Dhaneshwar, Shrishti Shandily, Vatsalya Tiwari
Endocrine, Metabolic & Immune Disorders - Drug Targets.2023; 23(6): 748. CrossRef - Revisiting the usefulness of the short acute octreotide test to predict treatment outcomes in acromegaly
Montserrat Marques-Pamies, Joan Gil, Elena Valassi, Marta Hernández, Betina Biagetti, Olga Giménez-Palop, Silvia Martínez, Cristina Carrato, Laura Pons, Rocío Villar-Taibo, Marta Araujo-Castro, Concepción Blanco, Inmaculada Simón, Andreu Simó-Servat, Gemm
Frontiers in Endocrinology.2023;[Epub] CrossRef - Evaluation and Management of Bone Health in Patients with Thyroid Diseases: a Position Statement from the Korean Thyroid Association
A Ram Hong, Hwa Young Ahn, Bu Kyung Kim, Seong Hee Ahn, So Young Park, Min-Hee Kim, Jeongmin Lee, Sun Wook Cho, Ho-Cheol Kang
International Journal of Thyroidology.2022; 15(1): 1. CrossRef - Octreotide in the treatment of acromegaly – the possibilities of high-dose therapy
I. A. Ilovayskaya
Meditsinskiy sovet = Medical Council.2022; (10): 148. CrossRef - Approach of Acromegaly during Pregnancy
Alexandru Dan Popescu, Mara Carsote, Ana Valea, Andreea Gabriela Nicola, Ionela Teodora Dascălu, Tiberiu Tircă, Jaqueline Abdul-Razzak, Mihaela Jana Țuculină
Diagnostics.2022; 12(11): 2669. CrossRef - Left to themselves: Time to target chronic pain in childhood rare diseases
Christine B. Sieberg, Alyssa Lebel, Erin Silliman, Scott Holmes, David Borsook, Igor Elman
Neuroscience & Biobehavioral Reviews.2021; 126: 276. CrossRef - Severe respiratory failure in a patient with COVID-19 and acromegaly: rapid improvement after adding octreotide
Jacob Luty, LesleAnn Hayward, Melanie Jackson, P Barton Duell
BMJ Case Reports.2021; 14(8): e243900. CrossRef - Precision Therapy in Acromegaly Caused by Pituitary Tumors: How Close Is It to Reality?
Cheol Ryong Ku, Vladimir Melnikov, Zhaoyun Zhang, Eun Jig Lee
Endocrinology and Metabolism.2020; 35(2): 206. CrossRef - Medical Treatment with Somatostatin Analogues in Acromegaly: Position Statement
Sang Ouk Chin, Cheol Ryong Ku, Byung Joon Kim, Sung-Woon Kim, Kyeong Hye Park, Kee Ho Song, Seungjoon Oh, Hyun Koo Yoon, Eun Jig Lee, Jung Min Lee, Jung Soo Lim, Jung Hee Kim, Kwang Joon Kim, Heung Yong Jin, Dae Jung Kim, Kyung Ae Lee, Seong-Su Moon, Dong
The Korean Journal of Medicine.2019; 94(6): 485. CrossRef
- Adrenal gland
- Effects of Altered Calcium Metabolism on Cardiac Parameters in Primary Aldosteronism
-
Jung Soo Lim, Namki Hong, Sungha Park, Sung Il Park, Young Taik Oh, Min Heui Yu, Pil Yong Lim, Yumie Rhee
-
Endocrinol Metab. 2018;33(4):485-492. Published online November 30, 2018
-
DOI: https://doi.org/10.3803/EnM.2018.33.4.485
-
-
4,066
View
-
43
Download
-
1
Web of Science
-
1
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
- Background
Increasing evidence supports interplay between aldosterone and parathyroid hormone (PTH), which may aggravate cardiovascular complications in various heart diseases. Negative structural cardiovascular remodeling by primary aldosteronism (PA) is also suspected to be associated with changes in calcium levels. However, to date, few clinical studies have examined how changes in calcium and PTH levels influence cardiovascular outcomes in PA patients. Therefore, we investigated the impact of altered calcium homeostasis caused by excessive aldosterone on cardiovascular parameters in patients with PA. MethodsForty-two patients (mean age 48.8±10.9 years; 1:1, male:female) whose plasma aldosterone concentration/plasma renin activity ratio was more than 30 were selected among those who had visited Severance Hospital from 2010 to 2014. All patients underwent adrenal venous sampling with complete access to both adrenal veins. ResultsThe prevalence of unilateral adrenal adenoma (54.8%) was similar to that of bilateral adrenal hyperplasia. Mean serum corrected calcium level was 8.9±0.3 mg/dL (range, 8.3 to 9.9). The corrected calcium level had a negative linear correlation with left ventricular end-diastolic diameter (LVEDD, ρ=−0.424, P=0.031). Moreover, multivariable regression analysis showed that the corrected calcium level was marginally associated with the LVEDD and corrected QT (QTc) interval (β=−0.366, P=0.068 and β=−0.252, P=0.070, respectively). ConclusionAldosterone-mediated hypercalciuria and subsequent hypocalcemia may be partly involved in the development of cardiac remodeling as well as a prolonged QTc interval, in subjects with PA, thereby triggering deleterious effects on target organs additively.
-
Citations
Citations to this article as recorded by  - Bone and mineral metabolism in patients with primary aldosteronism: A systematic review and meta-analysis
Anning Wang, Yuhan Wang, Hongzhou Liu, Xiaodong Hu, Jiefei Li, Huaijin Xu, Zhimei Nie, Lingjing Zhang, Zhaohui Lyu
Frontiers in Endocrinology.2022;[Epub] CrossRef
- Clinical Guidelines for the Management of Adrenal Incidentaloma
-
Jung-Min Lee, Mee Kyoung Kim, Seung-Hyun Ko, Jung-Min Koh, Bo-Yeon Kim, Sang Wan Kim, Soo-Kyung Kim, Hae Jin Kim, Ohk-Hyun Ryu, Juri Park, Jung Soo Lim, Seong Yeon Kim, Young Kee Shong, Soon Jib Yoo
-
Endocrinol Metab. 2017;32(2):200-218. Published online June 23, 2017
-
DOI: https://doi.org/10.3803/EnM.2017.32.2.200
-
-
16,178
View
-
688
Download
-
80
Web of Science
-
78
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader
An adrenal incidentaloma is an adrenal mass found in an imaging study performed for other reasons unrelated to adrenal disease and often accompanied by obesity, diabetes, or hypertension. The prevalence and incidence of adrenal incidentaloma increase with age and are also expected to rise due to the rapid development of imaging technology and frequent imaging studies. The Korean Endocrine Society is promoting an appropriate practice guideline to meet the rising incidence of adrenal incidentaloma, in cooperation with the Korean Adrenal Gland and Endocrine Hypertension Study Group. In this paper, we discuss important core issues in managing the patients with adrenal incidentaloma. After evaluating core proposition, we propose the most critical 20 recommendations from the initially organized 47 recommendations by Delphi technique. -
Citations
Citations to this article as recorded by  - The improvement of postoperative blood pressure and associated factors in patients with hormone‐negative adrenal adenoma and hypertension
Jiaxing Sun, Yingchun Dong, Hanbo Wang, Xudong Guo, Ning Suo, Shangjian Li, Xiangbin Ren, Shaobo Jiang
Journal of Surgical Oncology.2024; 129(6): 1073. CrossRef - Clinical features and treatment options for pediatric adrenal incidentalomas: a retrospective single center study
Xiaojiang Zhu, Saisai Liu, Yimin Yuan, Nannan Gu, Jintong Sha, Yunfei Guo, Yongji Deng
BMC Pediatrics.2024;[Epub] CrossRef - Characterizing incidental mass lesions in abdominal dual-energy CT compared to conventional contrast-enhanced CT
Jack Junchi Xu, Peter Sommer Ulriksen, Camilla Wium Bjerrum, Michael Patrick Achiam, Timothy Andrew Resch, Lars Lönn, Kristoffer Lindskov Hansen
Acta Radiologica.2023; 64(3): 945. CrossRef - Metastatic Adrenal PEComa: Case Report and Short Review of the Literature
Enrico Battistella, Luca Pomba, Marica Mirabella, Michele Gregianin, Antonio Scapinello, Marco Volante, Antonio Toniato
Medicina.2023; 59(1): 149. CrossRef - Surgical management and outcomes of spinal metastasis of malignant adrenal tumor: A retrospective study of six cases and literature review
Xiangzhi Ni, Jing Wang, Jiashi Cao, Kun Zhang, Shuming Hou, Xing Huang, Yuanjin Song, Xin Gao, Jianru Xiao, Tielong Liu
Frontiers in Oncology.2023;[Epub] CrossRef - An adrenal incidentaloma that had appeared to produce dehydroepiandrosterone-sulfate in excess before immunohistochemical study of the tumor
Toshihide Yamamoto, Takuma Kimura, Yuki Kubo, Shin-ichi Nakatsuka, Hiromasa Harada, Takashi Suzuki, Hironobu Sasano
Endocrine Journal.2023; 70(1): 43. CrossRef - Mortality Not Increased in Patients With Nonfunctional Adrenal Adenomas: A Matched Cohort Study
Albin Kjellbom, Ola Lindgren, Malin Danielsson, Henrik Olsen, Magnus Löndahl
The Journal of Clinical Endocrinology & Metabolism.2023; 108(8): e536. CrossRef - Construction of a novel clinical nomogram to predict cancer-specific survival in patients with primary malignant adrenal tumors: a large population-based retrospective study
Mingzhen Li, Xiaoying Duan, Di You, Linlin Liu
Frontiers in Medicine.2023;[Epub] CrossRef - Primary Aldosteronism Prevalence – An Unfolding
Story
Suranut Charoensri, Adina F. Turcu
Experimental and Clinical Endocrinology & Diabetes.2023; 131(07/08): 394. CrossRef - Management of Adrenal Cortical Adenomas: Assessment of Bone Status in Patients with (Non-Functioning) Adrenal Incidentalomas
Alexandra-Ioana Trandafir, Mihaela Stanciu, Simona Elena Albu, Vasile Razvan Stoian, Irina Ciofu, Cristian Persu, Claudiu Nistor, Mara Carsote
Journal of Clinical Medicine.2023; 12(13): 4244. CrossRef - Clinical manifestations of functionally autonomous cortisol secretion in patients with adrenal masse
T. R. Chzhen, T. P. Kiseleva
Ural Medical Journal.2023; 22(3): 13. CrossRef - Tumor enlargement in adrenal incidentaloma is related to glaucoma: a new prognostic feature?
M. Caputo, T. Daffara, A. Ferrero, M. Romanisio, E. Monti, C. Mele, M. Zavattaro, S. Tricca, A. Siani, A. Clemente, C. Palumbo, S. De Cillà, A. Carriero, A. Volpe, P. Marzullo, G. Aimaretti, F. Prodam
Journal of Endocrinological Investigation.2023; 47(2): 377. CrossRef - Adrenal ganglioneuroma: Features and outcomes of cases series
Pei Li, Rongchang Zhang, Guang Wang, Jiongming Li
Asian Journal of Surgery.2023; 46(11): 5272. CrossRef - Recent Updates on the Management of Adrenal Incidentalomas
Seung Shin Park, Jung Hee Kim
Endocrinology and Metabolism.2023; 38(4): 373. CrossRef - Adrenal malakoplakia a rare lesion that mimics a neoplasm
Orión Erenhú Rodríguez González, Jesus Eduardo Osorio, Edgar Iván Bravo Castro
Urology Case Reports.2023; 51: 102568. CrossRef - LC-MS based simultaneous profiling of adrenal hormones of steroids, catecholamines, and metanephrines
Jongsung Noh, Chaelin Lee, Jung Hee Kim, Seung Woon Myung, Man Ho Choi
Journal of Lipid Research.2023; 64(11): 100453. CrossRef - Incidentaloma adrenal. Del hallazgo casual al diagnóstico definitivo
Mercedes Retamal Ortíz, Ana Belén Vicario Parada, Elena Vázquez Jarén
Actualización en Medicina de Familia.2023;[Epub] CrossRef - Diagnosis and management of adrenal incidentaloma: use of clinical judgment and evidence in dialog with the patient
Yusaku Yoshida, Kiyomi Horiuchi, Michio Otsuki, Takahiro Okamoto
Surgery Today.2023;[Epub] CrossRef - Can MDCT Enhancement Patterns Be Helpful in Differentiating Secretory from Non-Functional Adrenal Adenoma?
Svetlana Kocic, Vladimir Vukomanovic, Aleksandar Djukic, Jovica Saponjski, Dusan Saponjski, Vuk Aleksic, Vesna Ignjatovic, Katarina Vuleta Nedic, Vladan Markovic, Radisa Vojinovic
Medicina.2023; 60(1): 72. CrossRef - Computer-assisted Reporting and Decision Support Increases Compliance with Follow-up Imaging and Hormonal Screening of Adrenal Incidentalomas
Renata R. Almeida, Bernardo C. Bizzo, Ramandeep Singh, Katherine P. Andriole, Tarik K. Alkasab
Academic Radiology.2022; 29(2): 236. CrossRef - Incidental Adrenal Masses: Adherence to Guidelines and Methods to Improve Initial Follow-Up: A Systematic Review
Timothy Feeney, Andrea Madiedo, Philip E. Knapp, Avneesh Gupta, David McAneny, Frederick Thurston Drake
Journal of Surgical Research.2022; 269: 18. CrossRef - Incidental Adrenal Lesions May Not Always Require Further Imaging Work-up
Deborah A. Baumgarten
Radiology.2022; 302(1): 138. CrossRef - Adrenal Nodules Detected at Staging CT in Patients with Resectable Gastric Cancers Have a Low Incidence of Malignancy
Hae Young Kim, Won Chang, Yoon Jin Lee, Ji Hoon Park, Jungheum Cho, Hee Young Na, Hyungwoo Ahn, Sung Il Hwang, Hak Jong Lee, Young Hoon Kim, Kyoung Ho Lee
Radiology.2022; 302(1): 129. CrossRef - Management of incidental adrenal nodules: a survey of abdominal radiologists conducted by the Society of Abdominal Radiology Disease-Focused Panel on Adrenal Neoplasms
Michael T. Corwin, Nicola Schieda, Erick M. Remer, Elaine M. Caoili
Abdominal Radiology.2022; 47(4): 1360. CrossRef - Primary hyperaldosteronism: indications for screening
Novella M. Chikhladze
Terapevticheskii arkhiv.2022; 94(1): 107. CrossRef - Pathophysiological Link between Insulin Resistance and Adrenal Incidentalomas
Jordan A. Higgs, Alyssa P. Quinn, Kevin D. Seely, Zeke Richards, Shad P. Mortensen, Cody S. Crandall, Amanda E. Brooks
International Journal of Molecular Sciences.2022; 23(8): 4340. CrossRef - Can Radiomics Provide Additional Diagnostic Value for Identifying Adrenal Lipid-Poor Adenomas From Non-Adenomas on Unenhanced CT?
Binhao Zhang, Huangqi Zhang, Xin Li, Shengze Jin, Jiawen Yang, Wenting Pan, Xue Dong, Jin Chen, Wenbin Ji
Frontiers in Oncology.2022;[Epub] CrossRef - Adrenal Surgery in the Era of Multidisciplinary Endocrine Tumor
Boards
Costanza Chiapponi, Daniel Pinto Dos Santos, Milan Janis Michael Hartmann, Matthias Schmidt, Michael Faust, Roger Wahba, Christiane Josephine Bruns, Anne Maria Schultheis, Hakan Alakus
Hormone and Metabolic Research.2022; 54(05): 294. CrossRef - Optimal and novel imaging of the adrenal glands
Patrick J. Navin, Michael R. Moynagh
Current Opinion in Endocrinology, Diabetes & Obesity.2022; 29(3): 253. CrossRef - Adrenal Tumors in Young Adults: Case Reports and Literature Review
Małgorzata Zdrojewska, Emilia Mech-Siebieszuk, Renata Świątkowska-Stodulska, Bartosz Regent, Michał Kunc, Łukasz Zdrojewski, Krzysztof Sworczak
Medicina.2022; 58(6): 746. CrossRef - Incidence of malignancy in adrenal nodules detected on staging CTs of patients with potentially resectable colorectal cancer
Hae Young Kim, Yoon Jin Lee, Won Chang, Ji Hoon Park, Jungheum Cho, Hyeon Jeong Oh, Young Hoon Kim, Kyoung Ho Lee
European Radiology.2022; 32(12): 8560. CrossRef - Appendiceal Incidentalomas: Prevalence, Radiographic Characteristics, Management, and Outcomes
Adam Kelly, Stacy O’Connor, Diana Kane, Chiang-Ching Huang, Harveshp Mogal
Annals of Surgical Oncology.2022; 29(13): 8265. CrossRef - Laparoscopic large adrenal mass resection: why we should be more careful?
Mohsen Varyani, Mahmood Parvin, Hamidreza Akbari Gilani
African Journal of Urology.2022;[Epub] CrossRef - Serum Visfatin/NAMPT as a Potential Risk Predictor for Malignancy of Adrenal Tumors
Nadia Sawicka-Gutaj, Hanna Komarowska, Dawid Gruszczyński, Aleksandra Derwich, Anna Klimont, Marek Ruchała
Journal of Clinical Medicine.2022; 11(19): 5563. CrossRef - Application of radiomics in adrenal incidentaloma: a literature review
Cheng Li, Yan Fu, Xiaoping Yi, Xiao Guan, Longfei Liu, Bihong T. Chen
Discover Oncology.2022;[Epub] CrossRef - Hormone-inactive adrenal tumors in clinician’s practice
T. R. Chzhen, T. P. Kiseleva
Perm Medical Journal.2022; 39(5): 48. CrossRef - The diagnostic value of salivary cortisol and salivary cortisone in patients with suspected hypercortisolism
Vendela Berndt, Per Dahlqvist, Jennie de Verdier, Henrik Ryberg, Oskar Ragnarsson
Frontiers in Endocrinology.2022;[Epub] CrossRef - The Role of Intraoperative Indocyanine Green (ICG) and Preoperative 3-Dimensional (3D) Reconstruction in Laparoscopic Adrenalectomy: A Propensity Score-matched Analysis
Giuseppe Palomba, Vincenza Paola Dinuzzi, Francesca Pegoraro, Roberto Ivan Troisi, Roberto Montalti, Giovanni Domenico De Palma, Giovanni Aprea
Surgical Laparoscopy, Endoscopy & Percutaneous Techniques.2022; 32(6): 643. CrossRef - The Etiological Profile of Adrenal Incidentalomas
Fatima-Zahra Lahmamssi, Loubna Saadaoui, Hayat Aynaou, Houda Salhi, Hanan El Ouahabi
Cureus.2022;[Epub] CrossRef - Forty Years Together, New Leap Forward! The 40th Anniversary of the Korean Endocrine Society
Jong Chul Won, Ki-Hyun Baek
Endocrinology and Metabolism.2022; 37(6): 851. CrossRef - Conduite à tenir face à un fortuitome surrénalien chez le chien ou le chat
Diane Pichard, Ghita Benckekroun
Le Nouveau Praticien Vétérinaire canine & féline.2022; 19(82): 40. CrossRef - Laparoscopic transperitoneal adrenalectomy: a comparative study of different techniques for vessel sealing
Luca Cardinali, Edlira Skrami, Elisa Catani, Flavia Carle, Monica Ortenzi, Andrea Balla, Mario Guerrieri
Surgical Endoscopy.2021; 35(2): 673. CrossRef - Epidemiology and Comorbidity of Adrenal Cushing Syndrome: A Nationwide Cohort Study
Chang Ho Ahn, Jung Hee Kim, Man Young Park, Sang Wan Kim
The Journal of Clinical Endocrinology & Metabolism.2021; 106(3): e1362. CrossRef - Urine steroid profile as a new promising tool for the evaluation of adrenal tumors. Literature review
Marta Araujo-Castro, Pablo Valderrábano, Héctor F. Escobar-Morreale, Felicia A. Hanzu, Gregori Casals
Endocrine.2021; 72(1): 40. CrossRef - A Rare Neoplasm: Primary Adrenal Leiomyosarcoma
Jack T. Barnett, Christine W. Liaw, Reza Mehrazin
Urology.2021; 148: e11. CrossRef - Adrenal Ganglioneuroma Presenting as an Incidentaloma in an Adolescent Patient
Sonia G. Sharma, Steven N. Levine, Xin Gu
AACE Clinical Case Reports.2021; 7(1): 61. CrossRef - Feasibility of Iodine-131 6β-Methyl-Iodo-19 Norcholesterol (NP-59) Scintigraphy to Complement Adrenal Venous Sampling in Management of Primary Aldosteronism: A Case Series
Jeongmin Lee, Jeonghoon Ha, Sang-Kuon Lee, Hye Lim Park, Sung-Hoon Kim, Dong-Jun Lim, Jung Min Lee, Sang-Ah Chang, Moo Il Kang, Min-Hee Kim
International Journal of General Medicine.2021; Volume 14: 673. CrossRef - Best Achievements in Pituitary and Adrenal Diseases in 2020
Chang Ho Ahn, Jung Hee Kim
Endocrinology and Metabolism.2021; 36(1): 51. CrossRef - Adrenal surgery: Review of 35 years experience in a single centre
Enrico Battistella, Stefania Ferrari, Luca Pomba, Antonio Toniato
Surgical Oncology.2021; 37: 101554. CrossRef - Adrenocortical Carcinoma: A Case of Missed Diagnosis
Yusef Hazimeh, Carlie Sigel, Carsello Carie, Mathew Leinung, Zaynab Khalaf
Cureus.2021;[Epub] CrossRef - Imagerie fonctionnelle en endocrinologie : nouveaux paradigmes à l’horizon 2020
E. Marchal
Médecine Nucléaire.2021; 45(3): 158. CrossRef - Adrenal Incidentaloma
Caren G. Solomon, Electron Kebebew
New England Journal of Medicine.2021; 384(16): 1542. CrossRef - Can Hematological Parameters Play a Role in the Differential Diagnosis of Adrenal Tumors?
Mehmet Gürkan Arıkan, Göktan Altuğ Öz, Nur Gülce İşkan, Necdet Süt, İlkan Yüksel, Ersan Arda
Uro.2021; 1(2): 39. CrossRef - Incidental Adrenal Nodules
Daniel I. Glazer, Michael T. Corwin, William W. Mayo-Smith
Radiologic Clinics of North America.2021; 59(4): 591. CrossRef - Antioxidant Barrier and Oxidative Damage to Proteins, Lipids, and DNA/RNA in Adrenal Tumor Patients
Barbara Choromańska, Piotr Myśliwiec, Tomasz Kozłowski, Magdalena Łuba, Piotr Wojskowicz, Jacek Dadan, Hanna Myśliwiec, Katarzyna Choromańska, Anna Gibała, Anna Starzyńska, Małgorzata Żendzian-Piotrowska, Anna Zalewska, Mateusz Maciejczyk, Jos L. Quiles
Oxidative Medicine and Cellular Longevity.2021; 2021: 1. CrossRef - Laparoscopic Retroperitoneoscopic Removal of an Adrenal Hemangioma: a Case Report
Kristin McCoy, Katherine Howe, Daniel Tershak
Journal of Endocrine Surgery.2021; 21(3): 70. CrossRef - Metabolic Subtyping of Adrenal Tumors: Prospective Multi-Center Cohort Study in Korea
Eu Jeong Ku, Chaelin Lee, Jaeyoon Shim, Sihoon Lee, Kyoung-Ah Kim, Sang Wan Kim, Yumie Rhee, Hyo-Jeong Kim, Jung Soo Lim, Choon Hee Chung, Sung Wan Chun, Soon-Jib Yoo, Ohk-Hyun Ryu, Ho Chan Cho, A Ram Hong, Chang Ho Ahn, Jung Hee Kim, Man Ho Choi
Endocrinology and Metabolism.2021; 36(5): 1131. CrossRef - Cross-Talk Between Nitrosative Stress, Inflammation and Hypoxia-Inducible Factor in Patients with Adrenal Masses
Barbara Choromańska, Piotr Myśliwiec, Tomasz Kozłowski, Magdalena Łuba, Piotr Wojskowicz, Jacek Dadan, Hanna Myśliwiec, Katarzyna Choromańska, Katarzyna Makarewicz, Anna Zalewska, Mateusz Maciejczyk
Journal of Inflammation Research.2021; Volume 14: 6317. CrossRef - Cirugía laparoscópica en incidentaloma suprarrenal para el cirujano general: serie de casos
Martín Adrián Bolívar-Rodríguez, Marcel Antonio Cázarez-Aguilar, Pedro Alejandro Magaña-Zavala, Francisco Magaña-Olivas, José Martín Niebla-Moreno
Revista Mexicana de Cirugía Endoscópica.2021; 22(1): 8. CrossRef - Adrenal adenomas: what to do with them? Review 2
S. Rybakov
INTERNATIONAL JOURNAL OF ENDOCRINOLOGY (Ukraine).2021; 17(3): 241. CrossRef - Is Follow-up of Adrenal Incidentalomas Always Mandatory?
Giuseppe Reimondo, Alessandra Muller, Elisa Ingargiola, Soraya Puglisi, Massimo Terzolo
Endocrinology and Metabolism.2020; 35(1): 26. CrossRef - Imaging Findings of Primary Adrenal Leiomyosarcoma: A Case Report
Hye Ran Yoon, Dong Hee Park
Journal of the Korean Society of Radiology.2020; 81(2): 459. CrossRef - WFUMB position paper on the management incidental findings: adrenal incidentaloma
Christoph F. Dietrich, Jean Michel Correas, Yi Dong, Christian Nolsoe, Susan Campbell Westerway, Christian Jenssen
Ultrasonography.2020; 39(1): 11. CrossRef - A nationwide survey of adrenal incidentalomas in Japan: the first report of clinical and epidemiological features
Takamasa Ichijo, Hajime Ueshiba, Hajime Nawata, Toshihiko Yanase
Endocrine Journal.2020; 67(2): 141. CrossRef - Mimics, pitfalls, and misdiagnoses of adrenal masses on CT and MRI
Khaled M. Elsayes, Mohab M. Elmohr, Sanaz Javadi, Christine O. Menias, Erick M. Remer, Ajaykumar C. Morani, Akram M. Shaaban
Abdominal Radiology.2020; 45(4): 982. CrossRef - Adrenal Incidentaloma
Mark Sherlock, Andrew Scarsbrook, Afroze Abbas, Sheila Fraser, Padiporn Limumpornpetch, Rosemary Dineen, Paul M Stewart
Endocrine Reviews.2020; 41(6): 775. CrossRef - A Web Application for Adrenal Incidentaloma Identification, Tracking, and Management Using Machine Learning
Wasif Bala, Jackson Steinkamp, Timothy Feeney, Avneesh Gupta, Abhinav Sharma, Jake Kantrowitz, Nicholas Cordella, James Moses, Frederick Thurston Drake
Applied Clinical Informatics.2020; 11(04): 606. CrossRef - Presentation and outcome of patients with an adrenal mass: A retrospective observational study
Nadeema Rafiq, Tauseef Nabi, SajadAhmad Dar, Shahnawaz Rasool
Clinical Cancer Investigation Journal.2020; 9(5): 198. CrossRef - Evaluation of Functionality and Growth Rates in Adrenal Incidentalomas: Single Center Experience
Suna AVCI, Yüksel Aslı OZTURKMEN, Sayid ZUHUR, Gulkan OZKAN, Elif GUVEN, Nazan DEMİR, Yuksel ALTUNTAS
Phoenix Medical Journal.2020; 2(3): 125. CrossRef - Percutaneous Adrenal Radiofrequency Ablation: A Short Review for Endocrinologists
Byung Kwan Park
Endocrinology and Metabolism.2020; 35(4): 750. CrossRef - Autonomous cortisol secretion in adrenal incidentalomas
Marta Araujo-Castro, Miguel Antonio Sampedro Núñez, Mónica Marazuela
Endocrine.2019; 64(1): 1. CrossRef - Primary adrenal schwannoma: a series of 31 cases emphasizing their clinicopathologic features and favorable prognosis
Jun Zhou, Dandan Zhang, Wencai Li, Luting Zhou, Haimin Xu, Saifang Zheng, Chaofu Wang
Endocrine.2019; 65(3): 662. CrossRef - Challenging risk factors for right and left laparoscopic adrenalectomy: A single centre experience with 272 cases
Kadir Omur Gunseren, Mehmet Cagatay Cicek, Hakan Vuruskan, Yakup Kordan, Ismet Yavascaoglu
International braz j urol.2019; 45(4): 747. CrossRef - A case report on 111In chloride bone marrow scintigraphy in management of adrenal myelolipoma
Tatsuya Yamamoto, Mitsuru Koizumi, Atsushi Kohno, Noboru Numao, Kentaro Inamura
Medicine.2019; 98(8): e14625. CrossRef - PRACTICAL ASPECTS OF LAPAROSCOPIC ADRENALECTOMY IN CHILDREN WITH BENIGN ADRENAL TUMORS
I. V. Poddubny, R. S. Oganesyan, K. N. Tolstov, M. A. Kareva
Russian Journal of Pediatric Surgery.2019; 23(5): 248. CrossRef - Incidental neuroblastoma with bilateral retinoblastoma: what are the chances?
Kelsey Roelofs, Furqan Shaikh, William Astle, Brenda L. Gallie, Sameh E. Soliman
Ophthalmic Genetics.2018; 39(3): 410. CrossRef - Surgical Considerations in Subclinical Cushing’s Syndrome. When is it Time to Operate?
Alexander M. Nixon, C Aggeli, C Tserkezis, GN Zografos
Hellenic Journal of Surgery.2018; 90(1): 27. CrossRef - Adrenal incidentaloma – diagnostic and treating problem – own experience
Ryszard Pogorzelski, Krzysztof Celejewski, Sadegh Toutounchi, Ewa Krajewska, Tomasz Wołoszko, Małgorzata Szostek, Wawrzyniec Jakuczun, Patryk Fiszer, Małgorzata Legocka, Zbigniew Gałązka
Open Medicine.2018; 13(1): 281. CrossRef
- Clinical Study
- Cardiac Dysfunction in Association with Increased Inflammatory Markers in Primary Aldosteronism
-
Jung Soo Lim, Sungha Park, Sung Il Park, Young Taik Oh, Eunhee Choi, Jang Young Kim, Yumie Rhee
-
Endocrinol Metab. 2016;31(4):567-576. Published online November 3, 2016
-
DOI: https://doi.org/10.3803/EnM.2016.31.4.567
-
Correction in: Endocrinol Metab 2020;35(3):671
-
5,376
View
-
43
Download
-
15
Web of Science
-
12
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader
- Background
Oxidative stress in primary aldosteronism (PA) is thought to worsen aldosterone-induced damage by activating proinflammatory processes. Therefore, we investigated whether inflammatory markers associated with oxidative stress is increased with negative impacts on heart function as evaluated by echocardiography in patients with PA. MethodsThirty-two subjects (mean age, 50.3±11.0 years; 14 males, 18 females) whose aldosterone-renin ratio was more than 30 among patients who visited Severance Hospital since 2010 were enrolled. Interleukin-1β (IL-1β), IL-6, IL-8, monocyte chemoattractant protein 1, tumor necrosis factor α (TNF-α), and matrix metalloproteinase 2 (MMP-2), and MMP-9 were measured. All patients underwent adrenal venous sampling with complete access to both adrenal veins. ResultsOnly MMP-2 level was significantly higher in the aldosterone-producing adenoma (APA) group than in the bilateral adrenal hyperplasia (BAH). Patients with APA had significantly higher left ventricular (LV) mass and A velocity, compared to those with BAH. IL-1β was positively correlated with left atrial volume index. Both TNF-α and MMP-2 also had positive linear correlation with A velocity. Furthermore, MMP-9 showed a positive correlation with LV mass, whereas it was negatively correlated with LV end-systolic diameter. ConclusionThese results suggest the possibility that some of inflammatory markers related to oxidative stress may be involved in developing diastolic dysfunction accompanied by LV hypertrophy in PA. Further investigations are needed to clarify the role of oxidative stress in the course of cardiac remodeling.
-
Citations
Citations to this article as recorded by  - 2023 Korean Endocrine Society Consensus Guidelines for the Diagnosis and Management of Primary Aldosteronism
Jeonghoon Ha, Jung Hwan Park, Kyoung Jin Kim, Jung Hee Kim, Kyong Yeun Jung, Jeongmin Lee, Jong Han Choi, Seung Hun Lee, Namki Hong, Jung Soo Lim, Byung Kwan Park, Jung-Han Kim, Kyeong Cheon Jung, Jooyoung Cho, Mi-kyung Kim, Choon Hee Chung
Endocrinology and Metabolism.2023; 38(6): 597. CrossRef - The role of the mineralocorticoid receptor in immune cells in cardiovascular disease
Charlotte D. C. C. van der Heijden, Marlies Bode, Niels P. Riksen, Ulrich O. Wenzel
British Journal of Pharmacology.2022; 179(13): 3135. CrossRef - Prevalence and clinical characteristics of primary aldosteronism in a tertiary-care center in Korea
Minjae Yoon, Namki Hong, Jaehyung Ha, Chan Joo Lee, Cheol Ryong Ku, Yumie Rhee, Sungha Park
Hypertension Research.2022; 45(9): 1418. CrossRef - Functional Characteristic and Significance of Aldosterone-Producing Cell Clusters in Primary Aldosteronism and Age-Related Hypertension
Fatin Athirah Pauzi, Elena Aisha Azizan
Frontiers in Endocrinology.2021;[Epub] CrossRef - Aldosterone-Regulating Receptors and Aldosterone-Driver Somatic Mutations
Jung Soo Lim, Samuel W. Plaska, Juilee Rege, William E. Rainey, Adina F. Turcu
Frontiers in Endocrinology.2021;[Epub] CrossRef - Time-Dependent Risk of Atrial Fibrillation in Patients With Primary Aldosteronism After Medical or Surgical Treatment Initiation
Kyoung Jin Kim, Namki Hong, Min Heui Yu, Hokyou Lee, Seunghyun Lee, Jung Soo Lim, Yumie Rhee
Hypertension.2021; 77(6): 1964. CrossRef - Serum Matrix Metalloproteinases and Left Atrial Remodeling—The Hoorn Study
Pauline B. C. Linssen, Hans-Peter Brunner-La Rocca, Casper G. Schalkwijk, Joline W. J. Beulens, Petra J. M. Elders, Amber A. van der Heijden, Roderick C. Slieker, Coen D. A. Stehouwer, Ronald M. A. Henry
International Journal of Molecular Sciences.2020; 21(14): 4944. CrossRef - Endothelial Dysfunction in Primary Aldosteronism
Zheng-Wei Chen, Cheng-Hsuan Tsai, Chien-Ting Pan, Chia-Hung Chou, Che-Wei Liao, Chi-Sheng Hung, Vin-Cent Wu, Yen-Hung Lin
International Journal of Molecular Sciences.2019; 20(20): 5214. CrossRef - IL-6 trans-signalling contributes to aldosterone-induced cardiac fibrosis
Chia-Hung Chou, Chi-Sheng Hung, Che-Wei Liao, Lin-Hung Wei, Ching-Way Chen, Chia-Tung Shun, Wen-Fen Wen, Cho-Hua Wan, Xue-Ming Wu, Yi-Yao Chang, Vin-Cent Wu, Kwan-Dun Wu, Yen-Hung Lin
Cardiovascular Research.2018; 114(5): 690. CrossRef - European Heart Rhythm Association (EHRA) position paper on arrhythmia management and device therapies in endocrine disorders, endorsed by Asia Pacific Heart Rhythm Society (APHRS) and Latin American Heart Rhythm Society (LAHRS)
Bulent Gorenek, Giuseppe Boriani, Gheorge-Andrei Dan, Laurent Fauchier, Guilherme Fenelon, He Huang, Gulmira Kudaiberdieva, Gregory Y H Lip, Rajiv Mahajan, Tatjana Potpara, Juan David Ramirez, Marc A Vos, Francisco Marin, Carina Blomstrom-Lundqvist, Aldo
EP Europace.2018; 20(6): 895. CrossRef - Effects of Altered Calcium Metabolism on Cardiac Parameters in Primary Aldosteronism
Jung Soo Lim, Namki Hong, Sungha Park, Sung Il Park, Young Taik Oh, Min Heui Yu, Pil Yong Lim, Yumie Rhee
Endocrinology and Metabolism.2018; 33(4): 485. CrossRef - The mineralocorticoid receptor as a modulator of innate immunity and atherosclerosis
Charlotte D C C van der Heijden, Jaap Deinum, Leo A B Joosten, Mihai G Netea, Niels P Riksen
Cardiovascular Research.2018; 114(7): 944. CrossRef
- Obesity and Metabolism
- Optimal Candidates for the Switch from Glimepiride to Sitagliptin to Reduce Hypoglycemia in Patients with Type 2 Diabetes Mellitus
-
Hyun Min Kim, Jung Soo Lim, Byung-Wan Lee, Eun-Seok Kang, Hyun Chul Lee, Bong-Soo Cha
-
Endocrinol Metab. 2015;30(1):84-91. Published online March 27, 2015
-
DOI: https://doi.org/10.3803/EnM.2015.30.1.84
-
-
5,854
View
-
98
Download
-
12
Web of Science
-
11
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader
- Background
Sitagliptin is a novel antidiabetic agent with a low risk for hypoglycemia. We investigated the efficacy and safety of sitagliptin when patients switched from a sulfonylurea to sitagliptin and identified good candidates for the switch. MethodsSixty-one patients with type 2 diabetes switched from glimepiride with metformin to sitagliptin with metformin due to clinical hypoglycemia. Serum glycated hemoglobin (HbA1c), fasting plasma glucose (FPG), and 2-hour postprandial plasma glucose (2h-PPG) before and 12 and 24 weeks after the drug switch were checked. ResultsHbA1c and FPG levels did not change 12 or 24 weeks after the switch; however, the 2h-PPG level decreased from 218.0±67.5 mg/dL at baseline to 197.1±69.9 mg/dL at 12 weeks and 192.3±67.4 mg/dL at 24 weeks after switching drugs (P=0.045, P=0.018, respectively). All but one patient no longer experienced hypoglycemia after discontinuing glimepiride. In a multivariate logistic regression analysis, a high homeostasis model assessment of insulin resistance and low baseline HbA1c level were independent predictors of an HbA1c ≤7% after switching to sitagliptin. ConclusionGlycemic control was not aggravated in patients 24 weeks after the drug switch, and symptomatic hypoglycemia decreased significantly. Patients with dominant insulin resistance may be good candidates for switching from a sulfonylurea to sitagliptin to reduce hypoglycemia.
-
Citations
Citations to this article as recorded by  - Application of Machine Learning Methods for the Development of Antidiabetic
Drugs
Juanjuan Zhao, Pengcheng Xu, Xiujuan Liu, Xiaobo Ji, Minjie Li, Dev Sooranna, Xiaosheng Qu, Wencong Lu, Bing Niu
Current Pharmaceutical Design.2022; 28(4): 260. CrossRef - Efficacy and safety of dorzagliatin for type 2 diabetes mellitus: A meta-analysis and trial sequential analysis
Yunfeng Yu, Xingyu Yang, Keke Tong, Shuang Yin, Gang Hu, Fei Zhang, Pengfei Jiang, Manli Zhou, Weixiong Jian
Frontiers in Cardiovascular Medicine.2022;[Epub] CrossRef - Factors associated with switching from sulphonylureas to dipeptidyl peptidase 4 inhibitors among patients with type 2 diabetes in the United States
Xi Tan, Lingfeng Yang, Kamlesh Khunti, Ruya Zhang, Ye Zhang, Swapnil Rajpathak, Miao Yu
Diabetes, Obesity and Metabolism.2021; 23(10): 2251. CrossRef - Increased risk of adverse cardiovascular events by strict glycemic control after percutaneous coronary intervention (HbA1c < 6.5% at 2 years) in type 2 diabetes mellitus combined with acute coronary syndrome: a 5-years follow-up study
Tiangui Yang, Peng Fu, Jie Chen, Xi Fu, Changlu Xu, Xiaoxia Liu, Tiesheng Niu
Current Medical Research and Opinion.2021; 37(9): 1517. CrossRef - Clinical analysis of pre-existing diabetes mellitus and dipeptidyl peptidase-4 inhibitors in patients with remitting seronegative symmetrical synovitis and pitting edema syndrome
Yoshiro Horai, Tomoki Origuchi, Nozomi Iwanaga, Junichi Tokumitsu, Toshiyuki Ikeoka, Genpei Kuriya, Yasumori Izumi, Atsushi Kawakami
Modern Rheumatology.2020; 30(4): 703. CrossRef - The efficacy and safety of dipeptidyl peptidase-4 inhibitors for type 2 diabetes: a Bayesian network meta-analysis of 58 randomized controlled trials
Juan Ling, Peng Cheng, Long Ge, Ding-hua Zhang, An-chen Shi, Jin-hui Tian, Ya-jing Chen, Xiu-xia Li, Jing-yun Zhang, Ke-hu Yang
Acta Diabetologica.2019; 56(3): 249. CrossRef - Satisfaction and efficacy of switching from daily dipeptidyl peptidase-4 inhibitors to weekly trelagliptin in patients with type 2 diabetes—Randomized controlled study—
Mayuko Oita, Hideaki Miyoshi, Kota Ono, Akinobu Nakamura, Kyu Yong Cho, Hiroshi Nomoto, Kohei Yamamoto, Kazuno Omori, Naoki Manda, Yoshio Kurihara, Shin Aoki, Tatsuya Atsumi
Endocrine Journal.2018; 65(2): 141. CrossRef - Efficacy and safety of evogliptin versus sitagliptin as add on to metformin alone in a combined russian-korean population. Evo-combi trial
Alina Y. Babenko, Anna A. Mosikian, Igor E. Makarenko, Victoriya V. Leusheva, Evgeny V. Shlyakhto
Diabetes mellitus.2018; 21(4): 241. CrossRef - Effectiveness prediction of Evogliptin treatment in type 2 diabetes mellitus in russian-korean population
Anna A. Mosikian, Alina Y. Babenko, Yulia A. Sevastyanova, Roman V. Drai, Evgenij V. Shlyakhto
Diabetes mellitus.2018; 21(5): 333. CrossRef - Comprehensive analysis of the Co-structures of dipeptidyl peptidase IV and its inhibitor
Hiroyuki Nojima, Kazuhiko Kanou, Genki Terashi, Mayuko Takeda-Shitaka, Gaku Inoue, Koichiro Atsuda, Chihiro Itoh, Chie Iguchi, Hajime Matsubara
BMC Structural Biology.2016;[Epub] CrossRef - A genetic variant in GLP1R is associated with response to DPP-4 inhibitors in patients with type 2 diabetes
Eugene Han, Hye Sun Park, Obin Kwon, Eun Yeong Choe, Hye Jin Wang, Yong-ho Lee, Sang-Hak Lee, Chul Hoon Kim, Lee-Kyung Kim, Soo Heon Kwak, Kyong Soo Park, Chul Sik Kim, Eun Seok Kang
Medicine.2016; 95(44): e5155. CrossRef
- A Case of Pituitary Adenoma with Simultaneous Secretion of TSH and GH.
-
Eun Young Lee, Cheol Ryong Ku, Hyun Min Kim, Woo Kyoung Lee, Jung Soo Lim, Sena Hwang, Do Hwan Kim, Dong Yeob Shin, Eun Jig Lee
-
Endocrinol Metab. 2011;26(2):160-165. Published online June 1, 2011
-
DOI: https://doi.org/10.3803/EnM.2011.26.2.160
-
-
2,959
View
-
30
Download
-
2
Crossref
-
 Abstract Abstract
 PDF PDF
- Thyrotropin (TSH)-secreting pituitary adenoma is a very rare disease. In one-quarter of patients suffering from this disease, the pituitary tumor secretes other anterior pituitary hormones. Herein, we report a case of pituitary adenoma with simultaneous secretion of TSH and growth hormone (GH). A 34-year-old female visitied local hospital complaining of sweating, intermittent palpitation, and weight loss of 8 kg within 1 year. The patient had undergone trans-sphenoidal surgery 3 years prior for resolution of a TSH and GH co-secreting pituitary adenoma. She had been administered somatostatin analogue prior to visiting our hospital. The patient's GH levels were suppressed to below 1 ng/mL on the 75 g oral glucose tolerance test, and her basal insulin-like growth factor-I (IGF-I) level was within normal range. Thyroid function tests demonstrated increased levels of both free thyroxine and TSH. Sella-MRI revealed pituitary adenoma at the floor of the pituitary fossa, approximately 2 cm in height. Therefore, she was diagnosed with residual TSH-secreting pituitary adenoma. The patient again underwent trans-sphenoidal surgery and entered complete remission, based on hormone levels and MRI findings.
-
Citations
Citations to this article as recorded by  - Endoscopic Transsphenoidal Surgery of Pituitary Adenomas: Preliminary Results of the Neurosurgery Service of Hospital Cristo Redentor
Gerson Perondi, Afonso Mariante, Fernando Azambuja, Gabriel Frizon Greggianin, Wanderson William dos Santos Dias, Giulia Pinzetta
Arquivos Brasileiros de Neurocirurgia: Brazilian Neurosurgery.2023; 42(02): e89. CrossRef - A case of a co-secreting TSH and growth hormone pituitary adenoma presenting with a thyroid nodule
Laura Hamilton Adams, Derick Adams
Endocrinology, Diabetes & Metabolism Case Reports.2018;[Epub] CrossRef
- Correlation between Pituitary Insufficiency and Magnetic Resonance Imaging Finding in Non-Functioning Pituitary Adenomas.
-
Hyun Min Kim, Cheol Ryong Ku, Eun Young Lee, Woo Kyung Lee, Jung Soo Lim, Sena Hwang, Mi Jung Lee, Seung Ku Lee, Sun Ho Kim, Eun Jig Lee
-
Endocrinol Metab. 2010;25(4):310-315. Published online December 1, 2010
-
DOI: https://doi.org/10.3803/EnM.2010.25.4.310
-
-
2,031
View
-
28
Download
-
1
Crossref
-
 Abstract Abstract
 PDF PDF
- BACKGROUND
Non-functioning pituitary adenomas (NFPAs) are characterized by the absence of clinical and biochemical evidence of pituitary hormone hypersecretion, and these tumors constitute approximately one third of all the tumors of the anterior pituitary. Recently, hormonal deficiencies have gradually evolved to become the leading presenting signs and symptoms in patients with NFPAs. We investigated pituitary hormonal insufficiencies according to the magnetic resonance imaging (MRI) findings in patients with NFPA. METHODS: We evaluated the patients who were newly diagnosed with NFPA from 1997 through 2009. Among them, we analyzed 387 patients who were tested for their combined pituitary function and who underwent MRI. The severity of the hypopituitarism was determined by the number of deficient axes of the pituitary hormones. On the MRI study, the maximal diameter of the tumor, Hardy's classification, the thickness of the pituitary gland and the presence of stalk compression were evaluated. RESULTS: The mean age was 46.85 +/- 12.93 years (range: 15-86) and 186 patients (48.1%) were male. As assessed on MRI, the tumor diameter was 27.87 +/- 9.93 mm, the thickness of the normal pituitary gland was 1.42 +/- 2.07 mm and stalk compression was observed in 201 patients (51.9%). Hypopituitarism was observed in 333 patients (86.0%). Deficiency for each pituitary hormone was most severe in the patients with Hardy type IIIA. Hypopituitarism was severe in the older age patients (P = 0.001) and the patients with a bigger tumor size (P < 0.001) and the presence of stalk compression (P < 0.001). However, the patients who had a thicker pituitary gland showed less severe hypopituitarism (P < 0.001). Multivariate analysis showed that age, tumor diameter and the thickness of pituitary gland were important determinants for pituitary deficiency (P = 0.004, P < 0.001, P = 0.022, respectively). CONCLUSION: The results suggest that the hormonal deficiencies in patient with NFPA were correlated with the MRI findings, and especially the tumor diameter and preservation of the pituitary gland.
-
Citations
Citations to this article as recorded by  - Clinical Parameters to Distinguish Silent Corticotroph Adenomas from Other Nonfunctioning Pituitary Adenomas
Daham Kim, Cheol Ryong Ku, Se Hee Park, Ju Hyung Moon, Eui Hyun Kim, Sun Ho Kim, Eun Jig Lee
World Neurosurgery.2018; 115: e464. CrossRef
|